What’s the Best Recurrent Yeast Infection Treatment?
Finding the best recurrent yeast infection treatment can be really difficult. In this article, I’ll help you find the most effective options that you can order online.
Vaginal yeast infections are very common among women and 75% of us will suffer from it at least once in our lifetime. Sometimes, yeast infections may become chronic and make your life a misery. You know you’re suffering from recurrent yeast infections if:
- You’ve had more than four vaginal yeast infections within a year
- Every time you had an infection you experience itching, redness, and discharge
- Your vaginal secretions have been examined by a doctor and Candida cultures have been found
- In some cases, especially if you self-diagnose, you may be suffering from a different kind of vaginal infection: Bacterial Vaginosis, or an STD. That’s why before starting your treatment it’s crucial to get tested. The easiest way is to order a Vaginal Health Test Kit online and get lab-certified results within days.

Once you’re sure it’s a yeast infection, there are different options when it comes to treating a recurrent condition. In this article I’ll help you choose the best recurrent yeast infection treatment:
Monistat and Fluconazole
Insert Monistat-7 vaginal suppositories for seven consecutive nights. On the first day of treatment take 150mg of Diflucan, followed by another dose after 72 hours. Your doctor may also recommend taking 150mg of Diflucan for up to 6 months as maintenance treatment.
If this treatment doesn’t work, it could mean that you’re infected by a different strain of Candida, such as Candida glabrata or Candida tropicalis, instead of the most common one Candida albicans.
That’s why it’s really important to have your vaginal secretions tested to know for sure what kind of infection you’re dealing with. In case it turns out you’re suffering from an infection by azole-resistant strains (Candida glabrata or Candida tropicalis) your doctor may prescribe Nystatin or…
Boric Acid Suppositories
Boric acid has been shown to be very effective in persistent recurrent yeast infections caused by Candida strains resistant to the most common over the counter medications.
The treatment usually involves inserting one boric acid suppository for seven consecutive nights followed by one suppository a week for up to 6 months as maintenance treatment.
Although boric acid can occasionally cause unpleasant side effects, such as a burning sensation, it’s considered a safe and economical option when it comes to treating recurrent vaginal yeast infections. In my opinion, boric acid suppositories are the best recurrent yeast infection treatment you can get.
What are the causes of recurrent yeast infections?
The main cause is the wrong diagnosis. You may be treated for a yeast infection while in reality, you’re suffering from a bacterial infection or a sexually transmitted disease.
That’s why it’s really important not to self-diagnose and insist on having your vaginal secretions tested to know for sure what kind of infection you’re dealing with.
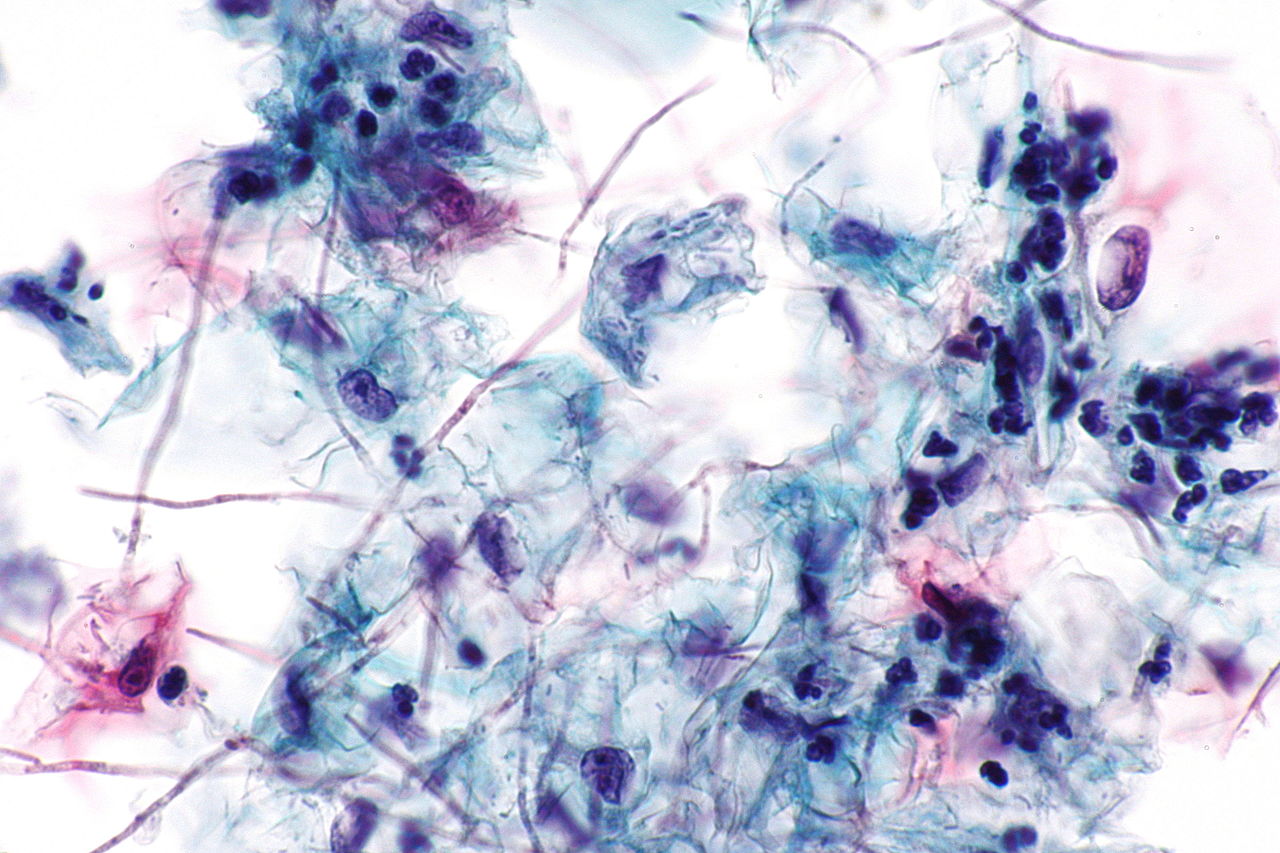
If you know for sure that you’re suffering from a yeast infection, the treatment works, but the infection keeps coming back, consider the following possible triggers of yeast infections and try to eliminate them:
- Taking antibiotics will increase your probabilities of developing a yeast infection. The matter with antibiotics is that they kill harmful microorganisms along with friendly bacteria making it easier for a fungus to multiply cause a yeast infection.
- Humidity and heat create perfect conditions for yeast to breed and cause nasty symptoms. To cut the risk of getting a yeast infection don’t wear tight, artificial underwear, tights, leggings, and trousers. In terms of fabric, your best choice is silk and cotton.
- Avoid wearing a wet swimsuit or sweaty clothes after a workout and change into dry clothes as soon as you can. Another nice tip is to sleep nude to keep your vaginal area dry and provide constant airflow to make it more difficult for yeast to breed.
- Alcohol disturbs the bacterial balance in your body, making it easier for the yeast to thrive. Whenever you drink, take probiotic suppositories or probiotic supplements to balance the number of friendly microorganisms in your body and boost your defenses against Candida.
- High levels of cortisol in your blood for a long period of time will weaken your immunity and make you more susceptible to vaginal yeast infection. Avoid situations that can expose you to chronic stress or practice relaxation techniques, such as meditation and yoga.
- Avoid foods that contain caffeine, such as chocolate or coffee to maintaining low levels of cortisol in your blood. Lack of sleep is another reason for heightened cortisol levels, so make getting enough sleep your priority.

- Studies show that if you have sex more than seven times per week it can cause small injuries to your vaginal area. These tiny wounds make you more susceptible to infection as they’re ideal for a fungus to grow. Remember that any kind of wound or injury within your vagina is an ideal place for Candida to breed causing an infection.
- Some condoms and sexual lubricants contain a spermicide know as nonoxynol-9. It’s also used in diaphragm jelly, cervical caps, and contraceptive sponges. Research shows that nonoxynol-9 can cause vaginal yeast infections, and make you more prone to catching HIV and other sexually transmitted diseases. Just make sure to check the ingredients in the above products before you purchase. Most brands, such as Durex don’t use nonoxynol-9 in their products anymore, but there are still some manufacturers who use it.

- You may be getting yeast infections because of hormonal changes that happen around your period or during pregnancy. You can prevent it by taking probiotic supplements that will help establish a healthy vaginal pH creating unfavorable conditions for yeast. You can also use probiotic tampons during your period to provide probiotics straight to your vagina so they can easily colonize it and make you more immune to infections.
- If you’re taking steroid medications you may be more prone to yeast infections. Ask your doctor to prescribe an oral antifungal medication, such as Diflucan, along with steroid medications, to prevent an infection. Diflucan taken once a week is a very effective preventative measure, another great option are boric acid suppositories inserted once a week.
- Avoid scented soaps and synthetic sexual lubricants, they can alter your vaginal pH and irritate the delicate vaginal tissues providing a perfect environment for yeast to thrive. Always try to choose 100% natural feminine washes and lubricants, that will not only be delicate but also provide antifungals, such as tea tree oil or coconut oil, helping you prevent future infections.

- Birth control pills with high estrogen levels can be the cause of recurrent yeast infections. If you feel that contraceptive pills could be triggering your infections, ask your doctor to prescribe you progestin-only pills or consider other methods of contraception.
- Swimming in chemically sanitized water found in most swimming pools can change your vaginal pH creating favorable conditions for yeast to cause an infection. If you like swimming, try to find UV or ozone sanitized pool in your area and never walk around in a wet swimsuit as humidity and warmth help yeast thrive.

- Avoid vaginal douches. They can disturb your vaginal flora leading to yeast infections and bacterial vaginosis.
- Recurrent yeast infections may be due to diabetics, HIV or other immunosuppressive diseases. Make sure you do all the necessary tests to exclude this possibility.
How to prevent recurrent yeast infections?
Apart from trying to eliminate all the above causes of chronic yeast infections, you can do the following:
- Use one probiotic suppository a week for up to 6 months to maintain a healthy vaginal pH and prevent harmful yeast from spreading
- Take probiotic supplements every day for as long as you want to maintain a good bacterial balance throughout your body. Providing fresh friendly bacteria cultures every day will make it difficult for pathogenic yeast to feed and breed causing an infection
- After drinking a lot of alcohol or swimming in a swimming pool, make sure that you use a probiotic suppository to further boost your defenses
- If you tend to get yeast infections straight after your period, switch to probiotic tampons instead of using the normal ones.
Conclusion
Recurrent vaginal yeast infections can seriously affect your quality of life, it can also put a strain on your relationship. It’s very important to act when you experience your first symptoms to prevent the infection from getting more severe and more difficult to treat.
In my experience, the best recurrent yeast infection treatment is boric acid suppositories. This medication is not only very effective but also natural and the risk of side effects is low.
Buy Boric Acid Suppositories Today
Make sure you don’t self-diagnose and see your gynecologist straight away. Insist on having your vaginal fluid tested to eliminate the possibility of a different kind of infection.
Apart from that, there are many things you can do to avoid getting recurrent yeast infections after successful treatment, so never give up because the solution is around the corner!

I’d love to hear about your experiences. Please share your comments and questions in the comment section below.



